Your Iron infusion covered by insurance investment are ready. Iron infusion covered by insurance are a car that is most popular and liked by everyone now. You can Get the Iron infusion covered by insurance files here. Find and Download all royalty-free house.
If you’re looking for iron infusion covered by insurance images information related to the iron infusion covered by insurance topic, you have pay a visit to the right site. Our site always gives you suggestions for seeing the maximum quality video and image content, please kindly surf and locate more enlightening video content and images that match your interests.
Iron Infusion Covered By Insurance. Covered for treatment of chronic iron overload. My old insurance company which did not pay for the surgery did pay for my infusions. The referral process for infusion therapy care. Our infusion center is a convenient alternative from the hospital setting.
 Does Health Insurance Cover Iron Infusions All From not.tradecabinet.com
Does Health Insurance Cover Iron Infusions All From not.tradecabinet.com
Iv iron products are infused directly into the bloodstream in a form that is readily available to the bone marrow for rbc synthesis, resulting in an earlier correction of iron deficiency and anemia. It’s best to discuss cost with your healthcare provider’s office, as they would have better access to these. These medications are typically given at an infusion center. Your doctor or healthcare provider will refer you to option care health to receive home or alternate site infusion therapy. Our infusion center is a convenient alternative from the hospital setting. Any recipient who is deficient in iron and can’t take iron pills orally or who is unable to sufficiently absorb iron from and the oral source could get coverage under part b.
However, you must respect certain conditions in order to get the advantage of this coverage.
Medicare will consider payment for code 96523©, irrigation of implanted venous access device for drug delivery systems, if it is the only service provided that day. However, there were certains ones they wouldn�t pay for. Iron infusions and medicare coverage. Your doctor or healthcare provider will refer you to option care health to receive home or alternate site infusion therapy. Over all the infusion process was very easy and i even got 2 infusions in the hospital post delivery, and the most challenging part was to hold a new born with cannula deep in my vein. I�ve had 16 infusions since may and still my numbers do not hold.
 Source: mnc.cfbcmobile.org
Source: mnc.cfbcmobile.org
The beneficiary is still responsible for any copays or coinsurance. You may need an iv infusion if you can’t take the supplements orally or absorb the iron through the gut. Remicade® & iron infusion services. I wonder if the dr could reword why you need it and if a different infusion would be covered. Each costs about $0.46 to $0.55 per mg of iron.
 Source: bn.produksicetak.com
Source: bn.produksicetak.com
Physician obtains consent and bchs general consent form is signed by patient. The beneficiary is still responsible for any copays or coinsurance. Our infusion center is a convenient alternative from the hospital setting. This is what their policy says: You may need an iv infusion if you can’t take the supplements orally or absorb the iron through the gut.
 Source: oba.premiumvapecarts.com
Source: oba.premiumvapecarts.com
Is iron infusion covered by insurance? And i did not have any out of pocket as my insurance covered the full cost. Effective december 1, 2000, medicare covers sodium ferric gluconate complex in sucrose injection as a first line treatment of iron deficiency anemia when furnished intravenously to patients undergoing chronic hemodialysis who are receiving supplemental erythropoeitin therapy. Most drugs used in home infusion therapy are covered under medicare part b, but if you have a medicare part d prescription drug plan, it may pay for some infusion drugs. Because of this, iron infusions would likely be covered under your medical insurance and not your prescription insurance.
 Source: mnc.cfbcmobile.org
Source: mnc.cfbcmobile.org
I just got a denial letter. Iron infusions and medicare coverage. However, there were certains ones they wouldn�t pay for. Having insurance cover iron infusion can lower the cost of the overall procedure. Your copay, coinsurance, and any relevant deductibles can increase how much you pay.
 Source: d2.beynil.org
Source: d2.beynil.org
I wonder if the dr could reword why you need it and if a different infusion would be covered. Our infusion center is a convenient alternative from the hospital setting. I wonder if the dr could reword why you need it and if a different infusion would be covered. This is what their policy says: Covered for a patient who has (a) a permanent (ordinarily, at least 3 months) nonfunction or disease of the structures that normally permit food to patients who suffer from blood loss may also need an iv iron shot.
 Source: r2.whiteorchidkeywest.com
Source: r2.whiteorchidkeywest.com
Physician obtains consent and bchs general consent form is signed by patient. Austin gastroenterology provides infusion services for patients receiving remicade® and iron infusions. Remicade® & iron infusion services. I wonder if the dr could reword why you need it and if a different infusion would be covered. Having insurance cover iron infusion can lower the cost of the overall procedure.
 Source: lig.pathwaystocharacter.org
Source: lig.pathwaystocharacter.org
Patients who suffer from blood loss may also need an iv iron shot. My ferritin level is 5 and hemoglobin is just below normal. Most insurance companies support the costs and the patient will have to pay only around 20% of the estimates mentioned above. How much does medicare reimburse for iron infusions? Administered by an external infusion pump.
 Source: oba.premiumvapecarts.com
Source: oba.premiumvapecarts.com
Iron infusions aren’t medications you would fill at your local community pharmacy. Many insurance companies shoulder the expenses, with patients paying around 20 percent of the costs posted above, but you will need to meet certain criteria before they agree to the terms. Covered for treatment of chronic iron overload. Having insurance cover iron infusion can lower the cost of the overall procedure. Your doctor or healthcare provider will refer you to option care health to receive home or alternate site infusion therapy.
 Source: k7.rebecaclayflores.org
Source: k7.rebecaclayflores.org
Iron infusions and medicare coverage. Our infusion center is a convenient alternative from the hospital setting. Any recipient who is deficient in iron and can’t take iron pills orally or who is unable to sufficiently absorb iron from and the oral source could get coverage under part b. These medications are typically given at an infusion center. Iron infusions aren’t medications you would fill at your local community pharmacy.
 Source: renovohealth.net
Source: renovohealth.net
Morning, fasting serum iron, ferritin, tibc and %tsat should be obtained; And iv iron should be considered when oral iron is. I�ve had 16 infusions since may and still my numbers do not hold. Your copay, coinsurance, and any relevant deductibles can increase how much you pay. Most insurance companies support the costs and the patient will have to pay only around 20% of the estimates mentioned above.
 Source: lig.pathwaystocharacter.org
Source: lig.pathwaystocharacter.org
The cost of the entire procedure may be reduced for patients who have insurance that covers iron infusion. These medications are typically given at an infusion center. Will insurance cover iron infusions. Covered for a patient who has (a) a permanent (ordinarily, at least 3 months) nonfunction or disease of the structures that normally permit food to patients who suffer from blood loss may also need an iv iron shot. The referral process for infusion therapy care.
 Source: not.tradecabinet.com
Source: not.tradecabinet.com
Oral iron treatment if tolerated and safe should be considered for ferritin less than or equal to 75 μg/l; My ferritin level is 5 and hemoglobin is just below normal. How much does medicare reimburse for iron infusions? Each costs about $0.46 to $0.55 per mg of iron. Austin gastroenterology provides infusion services for patients receiving remicade® and iron infusions.
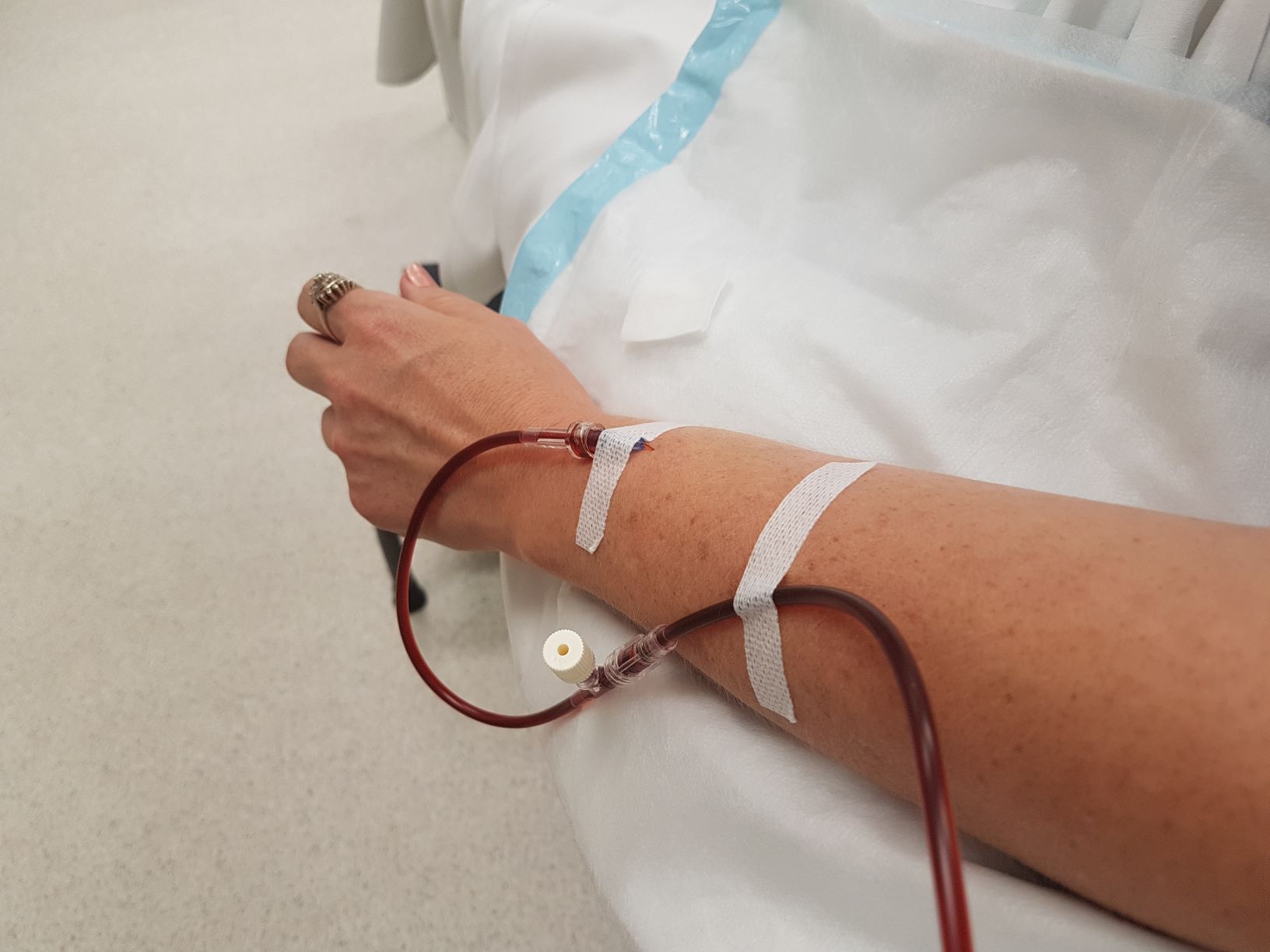 Source: bn.produksicetak.com
Source: bn.produksicetak.com
Each costs about $0.46 to $0.55 per mg of iron. Connect with a registration specialist. Most insurance companies support the costs and the patient will have to pay only around 20% of the estimates mentioned above. The cost of the entire procedure may be reduced for patients who have insurance that covers iron infusion. Have had iron infusions in the past covered by a different insurance.
 Source: not.tradecabinet.com
Source: not.tradecabinet.com
I just got a denial letter. Our infusion center is a convenient alternative from the hospital setting. About 9 million americans on medicare have gotten iron infusions each year since 2013, the first year for which data is available; Oral iron treatment if tolerated and safe should be considered for ferritin less than or equal to 75 μg/l; Indications and limitations of coverage.
 Source: oba.premiumvapecarts.com
Source: oba.premiumvapecarts.com
Physician obtains consent and bchs general consent form is signed by patient. Effective december 1, 2000, medicare covers sodium ferric gluconate complex in sucrose injection as a first line treatment of iron deficiency anemia when furnished intravenously to patients undergoing chronic hemodialysis who are receiving supplemental erythropoeitin therapy. Your doctor or healthcare provider will refer you to option care health to receive home or alternate site infusion therapy. Covered for treatment of chronic iron overload. Most drugs used in home infusion therapy are covered under medicare part b, but if you have a medicare part d prescription drug plan, it may pay for some infusion drugs.
 Source: tonsdart-news.blogspot.com
Source: tonsdart-news.blogspot.com
Medicare will consider payment for code 96523©, irrigation of implanted venous access device for drug delivery systems, if it is the only service provided that day. Will insurance cover iron infusions. Most iron infusions are done in an outpatient setting. Most insurance companies support the costs and the patient will have to pay only around 20% of the estimates mentioned above. Covered for a patient who has (a) a permanent (ordinarily, at least 3 months) nonfunction or disease of the structures that normally permit food to patients who suffer from blood loss may also need an iv iron shot.
 Source: mangga.icogovernance.org
Source: mangga.icogovernance.org
Patients who suffer from blood loss may also need an iv iron shot. You may need an iv infusion if you can’t take the supplements orally or absorb the iron through the gut. The beneficiary is still responsible for any copays or coinsurance. My old insurance company which did not pay for the surgery did pay for my infusions. I�ve had 16 infusions since may and still my numbers do not hold.
 Source: mnc.cfbcmobile.org
Source: mnc.cfbcmobile.org
And iv iron should be considered when oral iron is. Have had iron infusions in the past covered by a different insurance. Your copay, coinsurance, and any relevant deductibles can increase how much you pay. Having insurance cover iron infusion can lower the cost of the overall procedure. Because of this, iron infusions would likely be covered under your medical insurance and not your prescription insurance.
This site is an open community for users to submit their favorite wallpapers on the internet, all images or pictures in this website are for personal wallpaper use only, it is stricly prohibited to use this wallpaper for commercial purposes, if you are the author and find this image is shared without your permission, please kindly raise a DMCA report to Us.
If you find this site good, please support us by sharing this posts to your own social media accounts like Facebook, Instagram and so on or you can also bookmark this blog page with the title iron infusion covered by insurance by using Ctrl + D for devices a laptop with a Windows operating system or Command + D for laptops with an Apple operating system. If you use a smartphone, you can also use the drawer menu of the browser you are using. Whether it’s a Windows, Mac, iOS or Android operating system, you will still be able to bookmark this website.





