Your Does insurance cover cervical traction device infographic are ready. Does insurance cover cervical traction device are a risk that is most popular and liked by everyone this time. You can Get the Does insurance cover cervical traction device files here. Find and Download all free business.
If you’re searching for does insurance cover cervical traction device images information related to the does insurance cover cervical traction device interest, you have come to the right site. Our website frequently gives you suggestions for seeing the maximum quality video and picture content, please kindly surf and locate more enlightening video articles and images that match your interests.
Does Insurance Cover Cervical Traction Device. Depending on your plan, however, you may qualify for coverage. The equipment must be vital to your daily life, like an oxygen tank or blood sugar tests for diabetics, and not just for your comfort — like a humidifier or air purifier. Patients with health insurers who. The cervitrac is a revolutionary new neck brace that combines a decompression neck support with a traction device.
 MDS Cervitrac Cervical Traction Collar MDs Belt, Inc From mdsbelt.com
MDS Cervitrac Cervical Traction Collar MDs Belt, Inc From mdsbelt.com
Such conditions are a musculoskeletal or neurological impairment to qualify for a device. The beneficiary has a musculoskeletal or neurologic impairment requiring traction equipment; The saunders cervical traction device is also covered by most insurance companies, with written proof by a physical therapist or doctor stating that this type of home cervical traction treatment is medically necessary rather than clinical traction. Some insurance companies will pay or reimburse for the usage of a saunders cervical home traction device. We would like to show you a description here but the site won’t allow us. Most insurance companies are very specific regarding the conditions for which they will cover various types of cervical traction devices.
Covers traction equipment that your doctor prescribes for use in your home.
Cervical traction devices are covered under the durable medical equipment benefit (social security act §1861(s)(6)). Patients with health insurers who. The cervitrac by dds was recently approved to be covered by medicare and most private insurances this year. Cervical traction devices (e0840, e0849, e0850, e0855 and e0860) are covered only if both of the following criteria are met: Cervical traction devices are covered under the durable medical equipment benefit (social security act §1861(s)(6)). We would like to show you a description here but the site won’t allow us.
 Source: clinicalhealthservices.com
Source: clinicalhealthservices.com
Some insurance companies may cover the cost of a neck traction device, especially if your doctor has prescribed one for you. Medicare part b (medical insurance) part b covers certain doctors� services, outpatient care, medical supplies, and preventive services. Most insurance companies are very specific regarding the conditions for which they will cover various types of cervical traction devices. Others may only cover certain types of devices. At the current time, insurance companies and medicare do not have specific coverage for the restorex penile traction therapy device.
 Source: chartwelldms.com
Source: chartwelldms.com
At the current time, insurance companies and medicare do not have specific coverage for the restorex penile traction therapy device. Durable medical equipment (dme) is a device or tool that is medically necessary for a patient. For this reason, it’s best to speak directly to your insurance company to see what they will cover and what documentation is required in order to cover the device! Dme helps you with your illness, injury, or condition, and does not. Some health insurers like cigna consider home cervical and/or lumbar traction devices experimental, investigational or unproven and will not cover them for any indication.
 Source: ptandsr.com
Source: ptandsr.com
Others may only cover certain types of devices. With the cervitrac the user really can have it all. Others may only cover certain types of devices. To our knowledge, the saunders unit is covered by insurance. The way your relationship with your insurance company should work is:
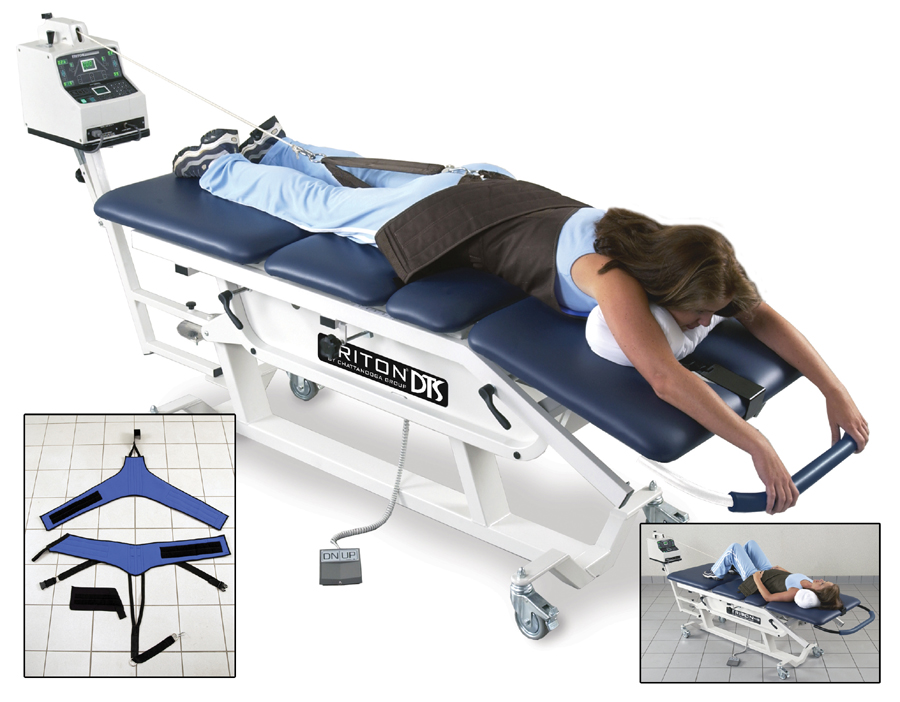 Source: trychiropracticfirst.com
Source: trychiropracticfirst.com
In order for a beneficiary�s dme to be eligible for reimbursement, the reasonable and necessary (r&n) requirements set out in the related local coverage determination must be met. The way your relationship with your insurance company should work is: The cervitrac by dds was recently approved to be covered by medicare and most private insurances this year. If you’ve recently had neck surgery, you shouldn’t use a neck traction device until you are fully recovered. Some insurance companies will pay or reimburse for the usage of a saunders cervical home traction device.
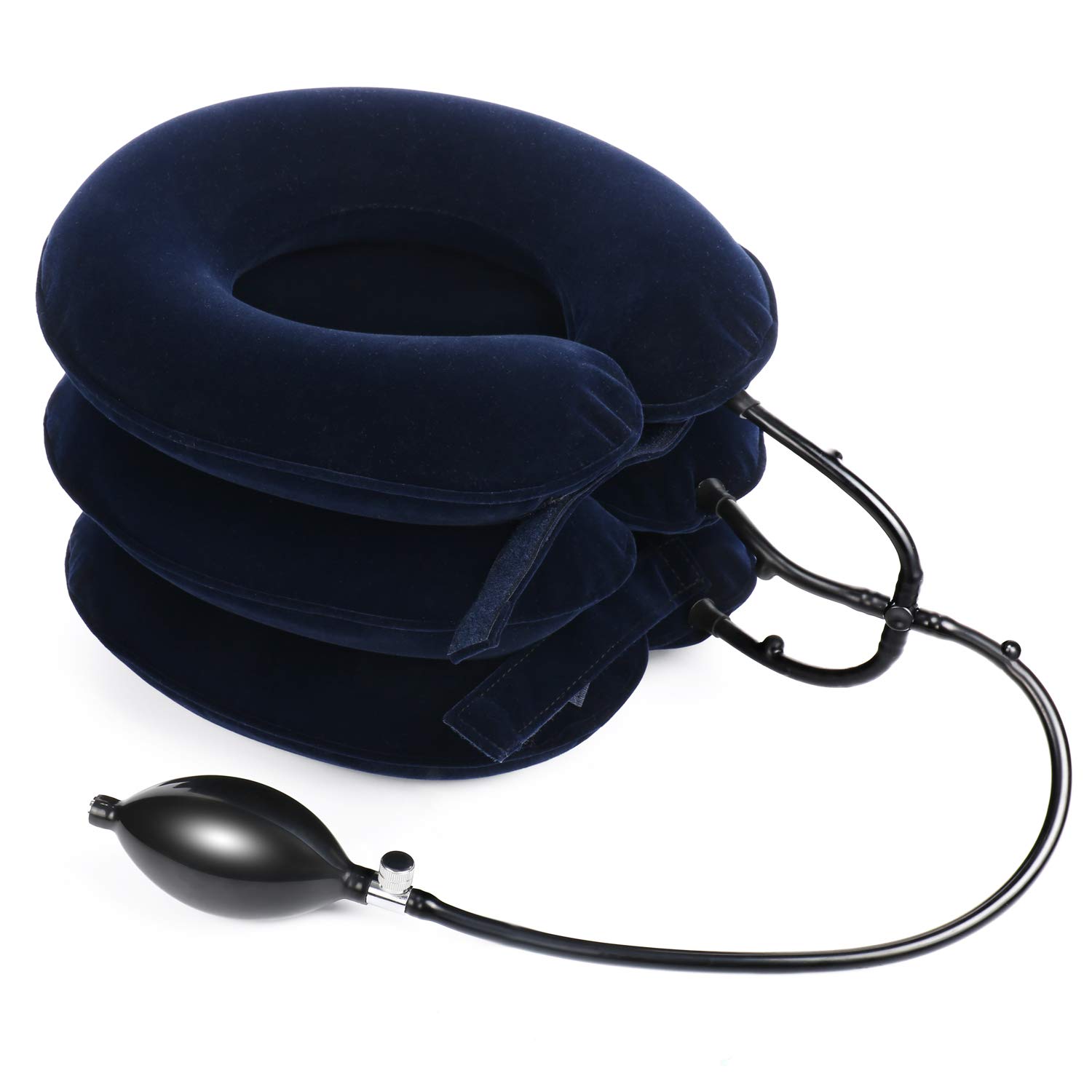 Source: amazon.com
Source: amazon.com
Some insurance companies will pay or reimburse for the usage of a saunders cervical home traction device. Patients with health insurers who. Cervical disc replacement is an alternative to cervical fusion surgery for treating pain, weakness or numbness in the neck or arms caused by severe degenerative disc disease in the cervical spine. Both you and your insurance company are bound by the terms of the agreement. Many men are receiving partial coverage for the restorex device.
 Source: medmassagerx.com
Source: medmassagerx.com
Cervical disc replacement is an alternative to cervical fusion surgery for treating pain, weakness or numbness in the neck or arms caused by severe degenerative disc disease in the cervical spine. The cervitrac is a revolutionary new neck brace that combines a decompression neck support with a traction device. For this reason, it’s best to speak directly to your insurance company to see what they will cover and what documentation is required in order to cover the device! We would like to show you a description here but the site won’t allow us. Depending on your plan, however, you may qualify for coverage.
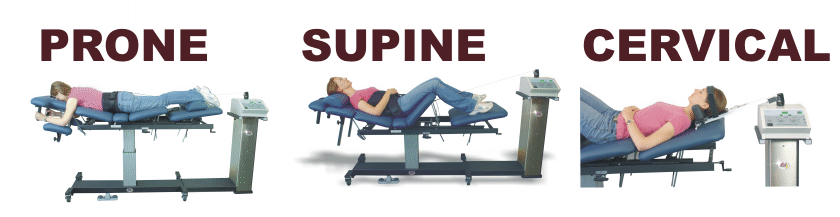
With the cervitrac the user really can have it all. Durable medical equipment (dme) is a device or tool that is medically necessary for a patient. Cervical traction devices are covered under the durable medical equipment benefit (social security act §1861(s)(6)). When filing for reimbursement, use the following: Refer to your specific health insurance policy to understand coverages related to payment and reimbursement of cervical artificial discs.
 Source: clinicalhealthservices.com
Source: clinicalhealthservices.com
When filing for reimbursement, use the following: The way your relationship with your insurance company should work is: Some insurance companies will pay or reimburse for the usage of a saunders cervical home traction device. Cervical disc replacement is an alternative to cervical fusion surgery for treating pain, weakness or numbness in the neck or arms caused by severe degenerative disc disease in the cervical spine. The equipment must be vital to your daily life, like an oxygen tank or blood sugar tests for diabetics, and not just for your comfort — like a humidifier or air purifier.
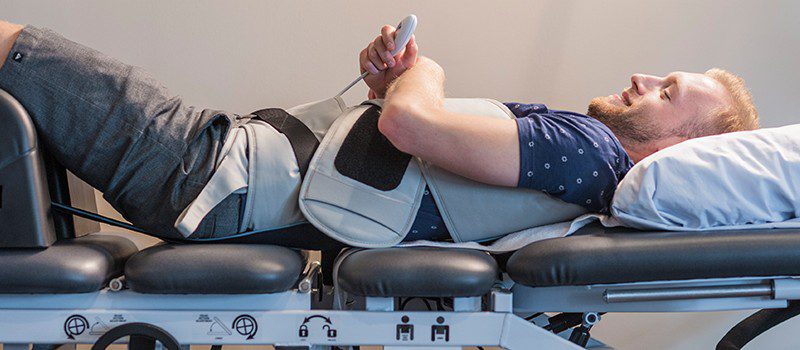 Source: leadingedgephysio.com
Source: leadingedgephysio.com
Cervical traction devices (e0840, e0849, e0850, e0855 and e0860) are covered only if both of the following criteria are met: The saunders cervical traction device is also covered by most insurance companies, with written proof by a physical therapist or doctor stating that this type of home cervical traction treatment is medically necessary rather than clinical traction. Cervical traction devices are covered under the durable medical equipment benefit (social security act §1861(s)(6)). Most insurance companies are very specific regarding the conditions for which they will cover various types of cervical traction devices. Code e0855 describes cervical traction devices that provide traction on the cervical anatomy without the use of a door or external frame or stand.
 Source: thecenteredstone.com
To our knowledge, the saunders unit is covered by insurance. Additionally, you must demonstrate that you can tolerate using the equipment. At the current time, insurance companies and medicare do not have specific coverage for the restorex penile traction therapy device. Depending on your plan, however, you may qualify for coverage. Cervical traction devices e0856 describes a cervical traction device that can be used with ambulation.
 Source: mdsbelt.com
Source: mdsbelt.com
Your doctor recommends a treatment or surgery. Durable medical equipment (dme) is a device or tool that is medically necessary for a patient. Although most insurance plans do cover traction (saunders cervical is a medicare covered benefit),clinicians can increase the likelihood of reimbursement by ensuring that the patient’s medical record contain items such as a description of the condition(s) that justify medical necessity for a traction device. If you’ve recently had neck surgery, you shouldn’t use a neck traction device until you are fully recovered. Cervical traction devices are covered under the durable medical equipment benefit (social security act §1861(s)(6)).
 Source: bidorbuy.co.za
Source: bidorbuy.co.za
If you’ve recently had neck surgery, you shouldn’t use a neck traction device until you are fully recovered. For this reason, it’s best to speak directly to your insurance company to see what they will cover and what documentation is required in order to cover the device! You can either call your insurance company in advance of ordering to determine your coverage […] For the purpose of this policy, traction is the use of a pulling force to treat muscle and or skeletal disorders of the spine. Constant traction resutls in tiring of the muscel s, allowing the strain to rest on the joint s.
 Source: blog.csamedicalsupply.com
Source: blog.csamedicalsupply.com
Code e0855 describes cervical traction devices that provide traction on the cervical anatomy without the use of a door or external frame or stand. Your doctor recommends a treatment or surgery. Patients with health insurers who. The equipment must be vital to your daily life, like an oxygen tank or blood sugar tests for diabetics, and not just for your comfort — like a humidifier or air purifier. Code e0855 describes cervical traction devices that provide traction on the cervical anatomy without the use of a door or external frame or stand.
 Source: pinterest.com
Source: pinterest.com
Most insurance companies are very specific regarding the conditions for which they will cover various types of cervical traction devices. Dds cervitrac cervical traction collar. Some health insurers like cigna consider home cervical and/or lumbar traction devices experimental, investigational or unproven and will not cover them for any indication. Refer to your specific health insurance policy to understand coverages related to payment and reimbursement of cervical artificial discs. If you’ve recently had neck surgery, you shouldn’t use a neck traction device until you are fully recovered.
 Source: kdimfg.com
Source: kdimfg.com
Code e0855 describes cervical traction devices that provide traction on the cervical anatomy without the use of a door or external frame or stand. Covers traction equipment that your doctor prescribes for use in your home. If you’ve recently had neck surgery, you shouldn’t use a neck traction device until you are fully recovered. Cervical traction cervical traction is noninvasive traction that is used to stretch the sof t tissues of the neck and to separate the spina ljoint structures to relieve neck pain. Additionally, you must demonstrate that you can tolerate using the equipment.
 Source: mdsbelt.com
Source: mdsbelt.com
Cervical traction devices e0856 describes a cervical traction device that can be used with ambulation. Dds cervitrac cervical traction collar. The saunders cervical traction device is also covered by most insurance companies, with written proof by a physical therapist or doctor stating that this type of home cervical traction treatment is medically necessary rather than clinical traction. Some insurance companies may cover the cost of a neck traction device, especially if your doctor has prescribed one for you. Therefore, it will be denied as not reasonable and necessary.
 Source: canyon-sports.com
Source: canyon-sports.com
Your doctor recommends a treatment or surgery. Some insurance companies may cover the cost of a neck traction device, especially if your doctor has prescribed one for you. Patients with health insurers who. Medicare part b (medical insurance) part b covers certain doctors� services, outpatient care, medical supplies, and preventive services. Constant traction resutls in tiring of the muscel s, allowing the strain to rest on the joint s.
 Source: openpr.com
Source: openpr.com
Many men are receiving partial coverage for the restorex device. Durable medical equipment (dme) is a device or tool that is medically necessary for a patient. Cervical disc replacement is an alternative to cervical fusion surgery for treating pain, weakness or numbness in the neck or arms caused by severe degenerative disc disease in the cervical spine. When filing for reimbursement, use the following: Dme helps you with your illness, injury, or condition, and does not.
This site is an open community for users to share their favorite wallpapers on the internet, all images or pictures in this website are for personal wallpaper use only, it is stricly prohibited to use this wallpaper for commercial purposes, if you are the author and find this image is shared without your permission, please kindly raise a DMCA report to Us.
If you find this site value, please support us by sharing this posts to your favorite social media accounts like Facebook, Instagram and so on or you can also save this blog page with the title does insurance cover cervical traction device by using Ctrl + D for devices a laptop with a Windows operating system or Command + D for laptops with an Apple operating system. If you use a smartphone, you can also use the drawer menu of the browser you are using. Whether it’s a Windows, Mac, iOS or Android operating system, you will still be able to bookmark this website.





